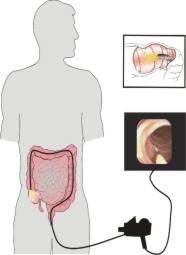
Under deep sedation a flexible colonoscope is used to examine the back passage, the large bowel and if possible the distal section of the small bowel. It is necessary to take a bowel preparation to clear the bowel so that good views are obtained of the mucosa. This examination is indicated for patients complaining of abdominal pain, change in bowel habit or blood loss from the gastrointestinal tract. It is a relatively safe procedure but significant problems such as bleeding or perforation (hole in the gut) may occur very rarely (less than one patient in one thousand). Severe anaesthetic complications occur rarely.
Sedation during Endoscopy
The most common type of anaesthetic technique used for endoscopies is “deep sedation”. The patient is deeply sedated but still conscious enough to breathe spontaneously. Sedative drugs are given through a cannula placed in a vein in the hand or arm. Occasionally patients may be aware of staff talking in the room but are not uncomfortable during the procedure. An anaesthetic spray may be used to numb the back of the throat. Sometimes, for instance with small children, it may be more appropriate to employ a “general anaesthetic” technique where breathing will be assisted and the airway protected from aspiration of gastric contents.
A pre-operative ECG may be required for certain patients. Close observation of the patient’s vital signs occurs peri operatively. A pulse oximeter will be used to monitor your pulse and the oxygen saturation in your blood. Deep sedation is generally very safe. Most serious anaesthetic problems occur in patients who already have a pre-existing illness or have a history of anaesthetic problems in the past.
Your anaesthetist will want to know:
- If you have fasted for your operation?
- Any adverse reactions to medications or pills?
- Any adverse reactions to previous anaesthetics?
- Medication you are taking at the moment?
- Any history of major medical problems?
- Any loose teeth, caps, crowns or dentures?
- If you are a smoker, if so when did you last smoke?
Common side effects (1 in 50 procedures) are bruising at the needle site, amnesia for a short time after the procedure and nausea. Less common side effects (1 in 100-1 in 5000) include severe vomiting, bruised or swollen lips, damage to teeth and headaches. Rare side effects (less than 1 in 5000) include aspiration (contents of stomach inhaled into lungs), severe allergic reaction and death. Cigarette smoking potentially increases the risks associated with anaesthesia and it is recommended that you stop smoking as long as possible before the procedure. Your anaesthetist will visit you in the Endoscopy Unit preoperative area prior to the procedure. Bring any concerns you may have to their attention.
Download the following pdf files if required.