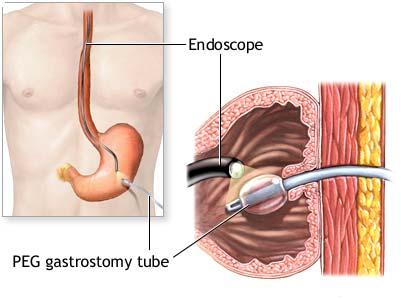
What is a PEG?
PEG stands for percutaneous (through the skin) endoscopic placement of tube (via an endoscope), gastrostomy (to the stomach). It is a procedure performed by a gastroenterologist (a specialist in digestive systems and related conditions), general surgeon or radiologist. It is a simple and safe way to receive food or drink when you cannot manage sufficient oral intake.
Special Considerations
The decision to proceed to a PEG tube is often not easy, particularly if the decision is being made on behalf of another person. The key question you will want to answer is “Will quality of life be improved with PEG feeding?” Close discussion with family members, nursing and medical staff and church contacts is often useful.
Aspirin and other anti-inflammatory (arthritis tablets) should be stopped 5-7 days prior to the procedure as they increase the risk of bleeding.
If you have diabetes, heart valve disease, a pacemaker implanted, or are taking blood-thinning tablets (eg Warfarin), it is important to discuss this with your doctor beforehand.
How is a PEG tube put in?
You need to have nothing to eat for 6 hours before the procedure and nothing to drink for 2 hours before the procedure. You may be given some antibiotics to reduce the risk of infection. Please tell your doctor if you are allergic to any particular antibiotic.
You will be given sedation by injection into a vein to make you feel more comfortable and your throat may be sprayed with a local anaesthetic. Children will usually require a general anaesthetic. A mouth guard is placed between your teeth to protect your teeth and the endoscope. Oxygen is given and your vital signs are closely monitored.
Lying comfortably on your side, the endoscope is passed via the mouth into the stomach. This instrument inspects the gullet and the stomach and the correct spot for the location of the tube is chosen. Local anaesthetic is injected into the skin and a small 1 cm cut is made in the skin of the upper abdomen. A flexible, hollow PEG tube is threaded inside the stomach leading out through the cut and the endoscope is then removed. The procedure usually takes 20-30 minutes.
What happens after the procedure?
All patients will recover from the sedation or anaesthesia in the hospital recovery area for at least 3-4 hours. Some patients may need to stay one or many nights after the procedure to recover and start a feeding regimen. If you are discharged that day you must NOT drive, ride, travel unaccompanied, operate machinery or sign legal documents on the day of the procedure. It is also advisable to have a friend or relative take you home and stay with you overnight.
Will I be in pain?
Your throat may be slightly sore for a few days after the procedure. The cut on your abdomen where the tube is inserted may be sore for up to a week. Simple oral analgesia such as Paracetemol, Tramadol or Codeine is usually adequate for pain relief.
Commencing feeding through the PEG
Feeds through the tube generally start with clear liquids between 6-24 hours after the procedure. Following this initial trial period you will be started on liquid nutritional supplements using a pump, large syringe or flask, depending on your preference. Your dietitian will advise on the type and quantity of feeds and full instruction and demonstration in feeding techniques will be given before discharge. Feeding pumps can be hired.
You may be able to continue to eat and drink by mouth in addition to using the PEG to complete your nutritional requirements. In some people the PEG tube will be necessary for all the feeding. Medications can also be given through the PEG tube but care is needed as some medications can set in the tubing. Your pharmacist can advise.
Are there any risks?
The insertion of a PEG tube is a safe procedure but complications can occur. There is a greater risk of complications if you are malnourished and it may be wise to have the PEG tube placed before too much weight is lost.
Minor complications occur in about 1 in 10 people. The most common is infection in the wound and uncommon events include leakage around the tube, nausea or vomiting for a few days or bleeding from the wound. Serious complications are rare. Death is a remote possibility with any endoscopic intervention.
PEG feeding usually gives great nutritional benefit although care must be taken with feeding to prevent feeds refluxing into the lungs and causing chest infections. The feeds must be stored correctly to prevent bacterial contamination.
What care does the PEG site need after the procedure?
Bathing with mild soap can start 24 hours after the PEG tube insertion. Dry around the PEG tube site and under the bolster/T bar after bathing. Keep this site clean and dry. The PEG tube should sit snugly against the skin and not cause any deep indentations. Rotate the tube full circle every day.
How long does the tube last?
Tubes can last up to a year, but sometimes tubes will need to be replaced earlier because they become clogged or perish. Occasionally the tube will accidentally fall out. A tube will need to be replaced within 24 hours to prevent the hole closing over. A temporary tube can be used if a dedicated PEG tube cannot be obtained. Any follow up or problems with the PEG should be referred to the Endoscopy Unit where the tube was inserted.
If a tube is no longer needed for feeding it can be simple removed (and the exit hole will quickly close over), although sometimes the removal will require another endoscopic procedure.
Download the following pdf file if required.